Coronary Angiography and Balloon–Stent Procedures in Coronary Artery Disease
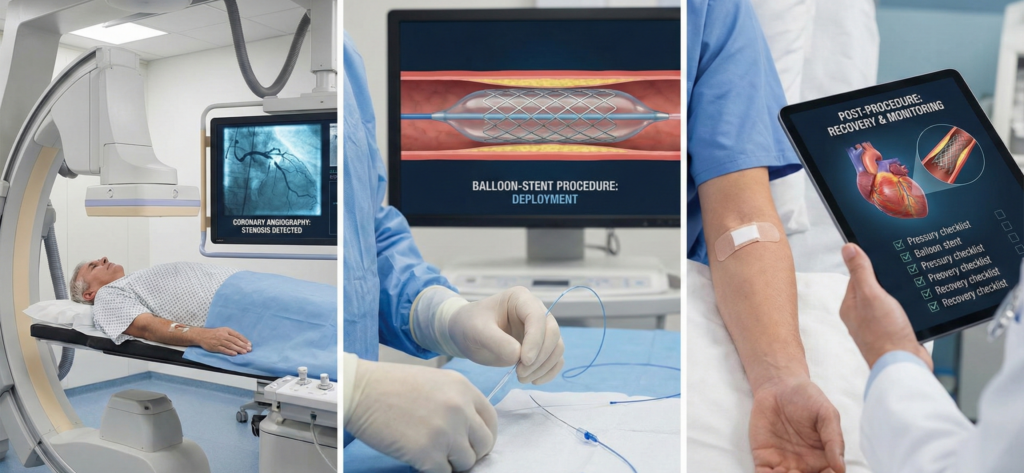
Coronary artery disease (CAD) refers to conditions in which the coronary arteries—responsible for supplying blood to the heart muscle—become narrowed or blocked, leading to partial or complete disruption of coronary blood flow.
Various tests are used in the diagnosis of CAD, including ECG, blood tests, exercise stress testing, echocardiography, nuclear cardiology imaging, magnetic resonance imaging, and multislice computed tomography. The diagnostic tool that best visualizes the coronary arteries is coronary angiography.
Following coronary angiography, treatment may consist solely of medication without further intervention. In suitable cases of narrowing or blockage, balloon angioplasty and/or stent placement can be performed, or coronary bypass surgery may be recommended. Balloon angioplasty–stenting procedures, performed through a percutaneous vascular access without surgery, are referred to as percutaneous coronary intervention (PCI). Approximately one-third of patients with coronary artery disease are treated with PCI.
Coronary stents were developed to overcome some of the limitations of balloon angioplasty and to achieve better blood flow through the opened artery. They have been widely used since the 1990s. A coronary stent (a metallic mesh scaffold) is used when balloon angioplasty alone cannot achieve adequate vessel patency or when tearing (dissection) occurs inside the vessel after balloon inflation. The stent is mounted on a balloon; when the balloon is inflated inside the artery, the stent expands and embeds into the vessel wall. Depending on the length of the narrowed area, one or more stents may be required. Within weeks, the stent becomes covered by endothelial tissue and remains in the artery for life.
With advances in stent technology, the need for bypass surgery has decreased to some extent. The success rate of balloon angioplasty and stenting ranges from 65% to 99%. Restenosis (re-narrowing) may occur in 20–30% of cases within six months. With drug-eluting stents, this risk decreases to 8–15%. If in-stent restenosis develops, repeat balloon angioplasty or placement of an additional stent may be performed.
What Are the Risks of These Procedures?
As with all interventional procedures, balloon angioplasty and stenting carry certain risks, although the complication rates are generally low.
Acute vessel closure, occurring during the procedure or within the first 24 hours, is a potential complication. However, this risk is significantly lower when a stent is placed. In stented patients, although the risk continues up to day 28, it decreases progressively. To minimize this risk, patients must take the antiplatelet (blood-thinning) medications prescribed by their physician.
Other potential complications include:
- Allergic reactions to local anesthetics or contrast dye
- Contrast-induced kidney dysfunction
- Excessive bleeding requiring surgery or blood transfusion
- Vascular injury at the access site caused by the catheter
- Embolization of blood clots from the heart or vessels leading to stroke
- Rare or previously undocumented adverse effects
Important Warning
After discharge from the hospital, patients should seek immediate medical attention if they develop:
- New or worsening chest pain
- Fever
- Shortness of breath
- Bleeding or a large swelling with discoloration at the vascular access site in the arm or leg
